Research into Parkinson’s disease continues to advance rapidly in 2026. While current therapies help alleviate symptoms, they cannot halt the progression of the disease – and many are associated with significant side effects. The good news is that several new therapeutic approaches are emerging that address this very issue and promise more.
In this three-part series, we present three novel Parkinson’s therapies that offer real cause for hope. In this first instalment, we focus on gene therapy – an approach that aims to protect vulnerable nerve cells and potentially slow the progression of the disease.
Gene therapy for Parkinson’s disease: a potentially disease-modifying approach
A gene therapy developed by AskBio (a subsidiary of Bayer AG) has been granted Regenerative Medicine Advanced Therapy (RMAT) designation by the US Food and Drug Administration (FDA) 1. This classification is reserved for innovative cell or gene therapies that have the potential to significantly alter the course of serious or life-threatening diseases – and signals strong regulatory support.
AskBio’s gene therapy, known as AB-1005, aims to slow the progression of Parkinson’s disease and improve motor function. An early clinical trial (Phase 1) showed that AB-1005 was well tolerated, with no serious product-related side effects.
How GDNF gene therapy works in Parkinson’s disease
In this study 2, 11 participants (8 men) aged between 35 and 75 received a single injection of GDNF (glial cell line-derived neurotrophic factor) – a protein that supports the growth of dopamine neurons – directly into the area of the brain affected by Parkinson’s disease, the putamen.
Participants were divided into two groups based on disease duration and MDS-UPDRS scores:
- Mild Parkinson’s disease: less than 5 years since clinical diagnosis; MDS-UPDRS Part 3 OFF score < 32
- Moderate Parkinson’s disease: 4 years or more since clinical diagnosis; MDS-UPDRS Part 3 OFF score 33–60
The primary objective of the study is to evaluate the safety and tolerability of GDNF infusion in individuals with mild to moderate Parkinson’s disease.
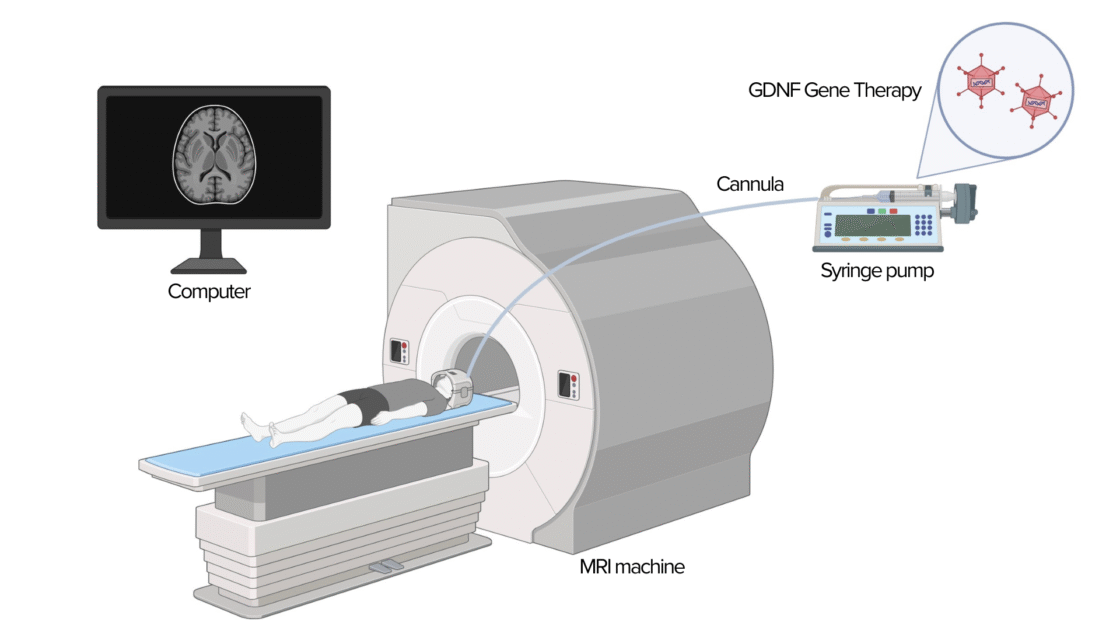
Safety and tolerability of GDNF gene therapy in Parkinson’s disease
All participants tolerated both the surgical procedure and the GDNF infusion well over an 18-month period following treatment. Some adverse effects occurred, but these subsided within 30 days of the injection. The most common symptoms included headaches, fatigue, tremors and chest pain.
During a routine MRI scan, researchers discovered cerebral ischaemia – a temporary reduction in blood flow, usually caused by a clot – near the injection site in one person. This is a known risk of such neurosurgical procedures, and all participants were informed about possible cerebrovascular events before being included in the study. The affected patient showed no symptoms, and the ischaemia remained stable during follow-up (up to 36 months).
Early clinical results: motor symptoms and medication requirements
Participants with moderate Parkinson’s disease showed improved motor control and required less daily levodopa. In addition, there were fewer instances of dyskinesia – involuntary movements often caused by Parkinson’s medication. Participants with mild Parkinson’s disease showed stable motor symptoms over 18 months after treatment, with only minor changes in their daily levodopa requirements.
What this gene therapy means for future Parkinson’s treatments
Taken together, these early results suggest that GDNF gene therapy could stabilise disease progression in people with mild Parkinson’s disease and restore dopamine-dependent brain activity in advanced disease. An ongoing Phase 2 trial, REGENERATE-PD, is currently investigating the sustainability and neuroprotective effects of this approach over a five-year period 3. Thanks to the RMAT designation, the therapy benefits from close monitoring by the FDA and the possibility of accelerated review, which means that important news could be available sooner than expected.

Stay tuned for Part 2, where we will focus on next-generation dopamine therapies designed to alleviate symptoms while reducing side effects. Sign up now for our Parkinson’s newsletter.
More about us
–> Back to the Parkinson’s Blog
References
- https://www.askbio.com/askbio-receives-fda-regenerative-medicine-advanced-therapy-designation-for-parkinsons-disease-investigational-gene-therapy/
- Van Laar AD, Christine CW, Phielipp N, et al. Intraputaminal Delivery of Adeno-Associated Virus Serotype 2-Glial Cell Line-Derived Neurotrophic Factor in Mild or Moderate Parkinson’s Disease. Mov Disord. 2025;40(7):1297-1306. doi:10.1002/mds.30193
- https://clinicaltrials.gov/study/NCT06285643
